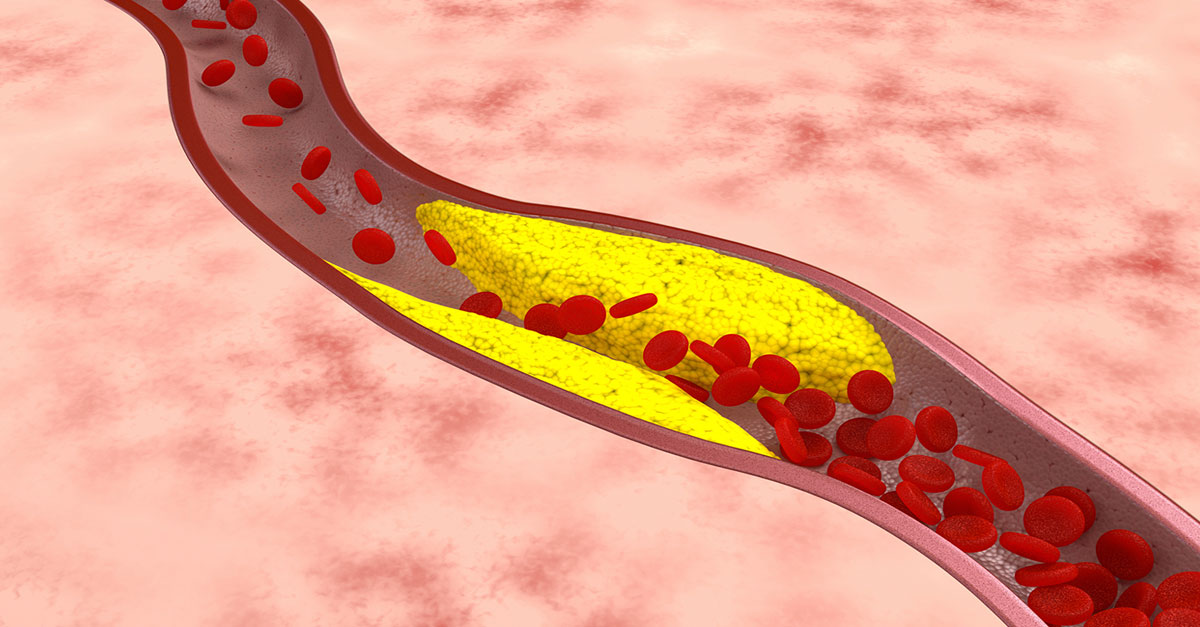
A fire could be smoldering inside your arteries…a type of fire that could erupt at any moment, triggering a heart attack or stroke. In fact, the fire could be building right this minute and you wouldn’t even know it. That’s because the usual things doctors look at when gauging cardiovascular risk—cholesterol, blood pressure, blood sugar, weight—can all appear to be fine even when your arteries are dangerously hot.
What does work to detect hot arteries? A set of six simple, inexpensive and readily available blood and urine tests. Problem: Few doctors order these tests, and few patients know enough to ask for them. Without the warnings these tests provide, patients often have no way of knowing just how great their risk is for heart attack or stroke and whether or not their preventive treatments are working—until it’s too late. Here’s how to protect yourself…
THE BODY’S ARMY ON ATTACK
Hot arteries are not actually hot (as in very warm)—instead, in this case “hot” refers to the effects of chronic inflammation. Why call them hot, then? “In this context, ‘hot’ is a perfect description,” said Bradley Bale, MD, medical director of the Grace Clinic Heart Health Program and an adjunct professor at Texas Tech Health Science Center, both in Lubbock, Texas. “Chronic arterial inflammation can put you on the fast track to developing vascular disease by speeding up the aging of your arteries. It’s so dangerous to the arterial lining that it’s worse than having high LDL cholesterol. And if your arteries are already clogged with plaque—which acts as kindling for a heart attack or stroke—inflammation is what lights the match.”
Inflammation in the body isn’t always bad, of course. In fact, it’s an important aspect of healing. When something in your body is under attack, the immune system sends in troops of white blood cells to repair and fight off the attacker, and temporary inflammation results. That’s why when you cut yourself, for example, you’ll see swelling at the site of the injury—it’s a sign that your white blood cells are at work for your benefit.
But: When an attack against your body persists (for instance, as occurs when you have an ongoing infection of the gums), your white blood cells continue to drive inflammation. When it turns chronic, inflammation becomes highly damaging to many tissues, including the arteries.
Normally, the endothelium (lining of the arteries) serves as a protective barrier between blood and the deeper layers of the arterial wall. However, when that lining is inflamed, it can’t function well and it gets sticky, almost like flypaper, trapping white blood cells on their way through the body, Dr. Bale said. The inflamed endothelium becomes leaky, too, allowing LDL “bad” cholesterol to penetrate into the wall of the artery. The white blood cells then gobble up the cholesterol, forming fatty streaks that ultimately turn into plaque, a condition called atherosclerosis. Then when the plaque itself becomes inflamed, it can rupture, tearing through the endothelium into the channel of the artery where blood flows. This material triggers the formation of a blood clot—a clot that could end up blocking blood flow to the heart or brain.
THE 6-PART FIRE PANEL
Just as firefighters have ways of determining whether a blaze is hiding within the walls of a building, certain tests can reveal whether inflammation is lurking within the walls of your arteries. With his own patients, Dr. Bale uses a set of six tests that he calls the “fire panel.” Each reveals different risk factors and, for several of the tests, too-high scores can have more than one cause—so it’s important to get all six tests, not just one or two, he said.
The fire panel can identify people at risk for developing atherosclerosis…reveal whether patients who already have atherosclerosis have dangerously hot arteries that could lead to a heart attack or stroke…and evaluate patients who have survived a heart attack or stroke to see whether their current treatments are working to reduce the inflammation that threatens their lives. Your individual test results will help determine your most appropriate course of treatment.
Dr. Bale recommends that all adults have this panel of tests done at least every 12 months—or every three to six months for patients at high risk for heart attack or stroke. All of these tests are readily available…are inexpensive and usually covered by insurance…and can be ordered by your regular doctor. Here are the six tests…
F2 Isoprostanes. Dr. Bale’s nickname for this blood test is the “lifestyle lie detector” because it reveals whether or not patients are practicing heart-healthy habits. The test, which measures a biomarker of oxidative stress, helps determine how fast your body’s cells are oxidizing, or breaking down. According to one study, people who have the highest levels of F2 isoprostanes are nine times more likely to have blockages in their coronary arteries than people with the lowest levels. The score you want: A normal score is less than 0.86 ng/L…an optimal score is less than 0.25 ng/L.
Fibrinogen. An abnormally high level of this sticky, fibrous protein in your blood can contribute to the formation of clots…it’s also a marker of inflammation. One study divided people into four groups (quartiles) based on their fibrinogen levels and found that stroke risk rose by nearly 50% for each quartile. High fibrinogen is particularly dangerous for people who also have high blood pressure because both conditions damage the blood vessel lining and make it easier for plaque to burrow inside, Dr. Bale said. Normal range: 440 mg/dL or lower.
High-Sensitivity C-Reactive Protein (hs-CRP). Your liver produces C-reactive protein, and the amount of it in your blood rises when there is inflammation in your body—so an elevated hs-CRP level generally is considered a precursor to cardiovascular disease. The large-scale Harvard Women’s Health Study cited this test as being more accurate than cholesterol in predicting risk for cardiovascular disease…while another study of women found that those with high scores were up to four times more likely to have a heart attack or stroke than women with lower scores. A high hs-CRP score is especially worrisome for a person with a large waist, according to Dr. Bale. Excess belly fat often is a sign of insulin resistance (in which cells don’t readily accept insulin), a condition that further magnifies heart attack and stroke risk. The score you’re aiming for: Under 1.0 mg/L is normal…0.5 mg/L is optimal.
Microalbumin/Creatinine Urine Ratio (MACR). This test looks for albumin in the urine. Albumin is a large protein molecule that circulates in the blood and shouldn’t spill from capillaries in the kidneys into the urine, so its presence suggests dysfunction of the endothelium. Though this test provides valuable information about arterial wall health, doctors rarely use it for this purpose. Important: New evidence shows that MACR levels that have traditionally been considered “normal” can signal increased risk for cardiovascular events, Dr. Bale cautioned. Optimal ratios, according to the latest research: 7.5 or lower for women and 4.0 or lower for men.
Lipoprotein-Associated Phospholipase A-2 (Lp-PLA2). This enzyme in the blood is attached to LDL cholesterol and rises when artery walls become inflamed. Recent research suggests that it plays a key role in the atherosclerosis disease process, contributing to the formation of plaque as well as to the plaque’s vulnerability to rupture, Dr. Bale said. People with periodontal (gum) disease are especially likely to have elevated Lp-PLA2 scores—chronic inflammation can start in unhealthy gums and, from there, spread to the arteries. Normal range: Less than 200 ng/mL.
Myeloperoxidase (MPO). This immune system enzyme normally is found at elevated levels only at the site of an infection. When it is elevated in the bloodstream, it must be assumed that it’s due to significant inflammation in the artery walls and leaking through the endothelium. This is a very bad sign. “MPO produces numerous oxidants that make all cholesterol compounds, including HDL ‘good’ cholesterol, more inflammatory. If your blood levels of MPO are high, HDL goes rogue and joins the gang of inflammatory thugs. It also interacts with another substance in the bloodstream to produce an acid that can eat holes in blood vessel walls,” Dr. Bale said. Smokers are particularly prone to high MPO levels. Normal range: Less than 420 pmol/L.
HOW TO PUT OUT THE FIRES
While the “fire panel” tests above may seem exotic, the solution to the hot artery problem, for most of us, is not. That’s because the best way to combat chronic inflammation is simply to maintain a healthful lifestyle, Dr. Bale said. You just have to do it! Key factors include…
• Following a heart-healthy Mediterranean-style diet.
• Managing stress.
• Getting plenty of exercise.
• Guarding against insulin resistance.
• Taking good care of your teeth and gums.
• Not smoking.
In some cases, lifestyle changes alone are enough to quell the flames of chronic inflammation and to put your arteries on the road to recovery. In other cases, patients also need medication such as statins and/or dietary supplements such as niacin and fish oil, Dr. Bale said. Either way, he added, “the good news is that once you shut the inflammation off, the body has a chance to heal whatever disease and damage has occurred—so you’re no longer on the fast track to a heart attack or stroke.”